The Smart Prosthesis Socket Liner
Actively monitored and controlled the pressure imparted on the user
Autonomously adapted its internal shape to fit the user
Monitored and lowered the temperature of the users limb
A soft, fabric-based pneumatic subsystem was developed to control the pressure imparted on the user. Six dependent soft pneumatic actuators were fabricated from nylon fabrics backed with thermoplastic polyurethane. A multi-input multi-output discrete controller was developed to control the pressure and the volume of each of the soft-pneumatic actuators in the socket liner. The closed-loop bandwidth of the pneumatic subsystem was adjustable depending on the provided source and sink pressure to and from the six soft-pneumatic actuators. The maximum bandwidth was characterized to be around 1 Hz.
Since the multi-input multi-output pneumatic control system was underactuated, the shape /geometry of the interface between the user and the socket liner was autonomously adaptable. The interface could adapt its shape and volume within 10% of the nominal limb volume in under 15 seconds. This was thought to extend time between prosthesis refitting. For pediatric patients, they need to be refitted for their prosthesis every 9-18 months until they reach adulthood. Additionally, this system allows for residual limb volume changes that can occur in adults over the course of the day due to hydration and activity.
Furthermore, a closed loop water cycle was used to dissipate heat produces by the user’s limb. Distilled water was forced through a fabric-based layer within the liner to absorb heat produced by the limb. After which, the water was pushed through a custom machined aluminum heat sink. A low-power 140 mm fan was used to force air thought the fins of the heat sink, dissipating the heat absorbed by the water. This 8 W subsystem was able to reduce the temperature of the human-socket interface by more than 2 degrees C.
Impedance Controlled Transradial Wearable
A 2-DOF robotic wearable was developed to vary the stiffness and damping between a user and the end-effector of the wearable, a laser pointer. This device was used to test how varying impedance of a human-wearable interface could affect participants’:
Tracking performance
Cognitive load
Perceptibility
A human subject study was carried out were more than 25 participants wore the wearable device four different impedance modes. The presentation order of the impedance settings was randomized for every participant. Each participant was tasked with tracking a moving target with the laser point on the wearable device. Computer vision techniques were used to determine their tracking performance. A pupillometry system was used to track the participants’ eye activity and pupil dilation over the course of every trial. Along with heartrate variability measures, the eye activity and pupillometry measurements were used to estimate the cognitive load induced by the tracking task and the impedance of the wearable. A dual task paradigm was also introduced were participants were tasked with answering verbal arithmetic questions (78-59) while they were tracking the targets. This induces more cognitive load and tested if the impedance of the wearable had an affect on the participants’ ability to perceive and respond to feedback.
For more information of the design and characterization of the wearable device please refer to the following publication. *
* A. B. Ambrose, C. VanAtter and F. L. Hammond, "An Impedance-Controlled Testbed for Simulating Variations in the Mechanical Fit of Wearable Devices," 2022 IEEE/RSJ International Conference on Intelligent Robots and Systems (IROS), Kyoto, Japan, 2022, pp. 9736-9743, doi: 10.1109/IROS47612.2022.9981391.
Depiction of the Semi-Active Wearable used to control the mechanical impedance between users’ forearms and laser pointer end-effector (A. Ambrose et al. 2022)
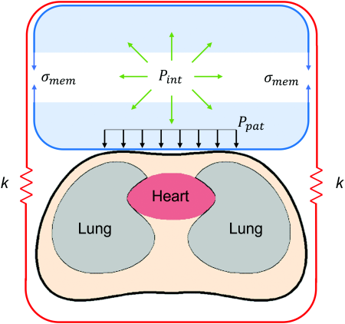
The Ventilation-Perfusion (V/Q) Vest
The ventilation-perfusion, V/Q Vest project started at the height of the COVID-19 pandemic. A new solution was sought to improve the oxygenation of patients suffering from acute respiratory distress syndrome (ARDS) caused by COVID-19. Even while on mechanical ventilators, patients with severe presentations of ARDS had diminished ability to absorb the oxygen provided (ventilation) into the bloodstream (perfusion). The V/Q vest was made to compress, in a controlled manner, the thoracic cavity of intubated patients. The compression caused a novel phenomenon, recruiting alveoli that were previously not participating in gas exchange. The result was an increase in the P/F ratio and the partial pressure of oxygen in patients’ bloodstreams.
The V/Q Vest was shown to predict how a patient will respond to proning, could be used to improve an intubated patient’s P/F similar to that of proning, and could be used on patients when proning was not a viable solution. This new treatment method could improve ARDS patient outcomes and provide an alternative pathway to risky and costly procedures, like using the Rotoprone and ECMO machines.
For more information, see the following publication of the V/Q Vest design and preclinical trials.*
* A. B. Ambrose, L. Tiziani, D. J. Ward, M. Weinmann, and F. L. Hammond, "A Pneumatic Compression Vest for Transthoracic Manipulation of Ventilation-Perfusion in Critical Care Patients with Acute Respiratory Distress Syndrome Caused by COVID-19." Proceedings of the 2021 Design of Medical Devices Conference. 2021 Design of Medical Devices Conference. Minneapolis, MN, USA. April 12–15, 2021. V001T04A007. ASME, doi: 10.1115/DMD2021-1056.
*A. B. Ambrose,J. F. Detelich, M. Weinmann, and F. L. Hammond, "Evaluation of a Pneumatic Vest to Treat Symptoms of ARDS Caused by COVID-19." ASME. J. Med. Devices. March 2022; 16(1): 011004, doi: 10.1115/1.4053387.
For more information about my graduate research, please visit the Adaptive Robotic Manipulation (ARM) lab website.